Sentinel events are serious, unexpected events that happen in hospitals or clinics. These events can cause severe harm or even death. Because they are so serious, healthcare organizations study them closely so they can prevent them from happening again. The purpose of identifying sentinel events is to identify ways to improve quality and reduce adverse events in healthcare settings.
Based on reports submitted to The Joint Commission in 2025, the most frequent types of sentinel events occurred in 2025 are estimated to be 1443 plus which are 8% lower than 1575 events occurred in 2024.
List of the Most Common Sentinel Events
According to the Joint Commission, the 1575 sentinel events reported in 2024 are:
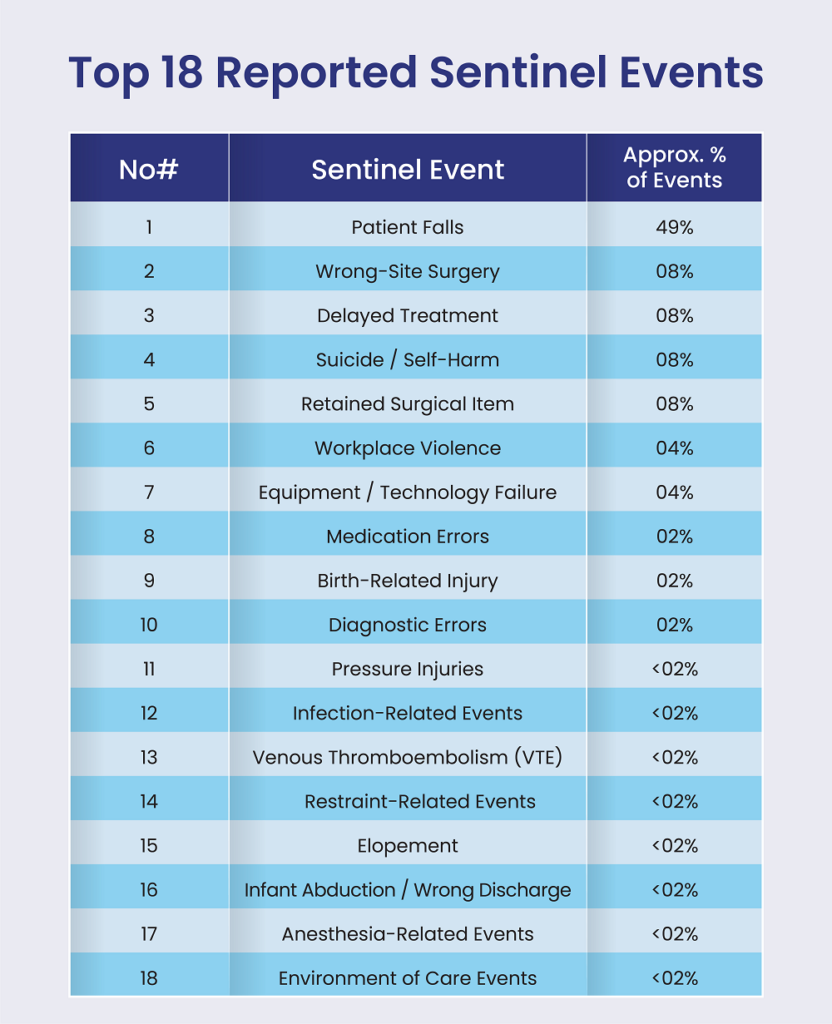
| # | Sentinel Event | Approx. % of Events |
| 1 | Patient Falls | 49% |
| 2 | Wrong-Site Surgery | 8% |
| 3 | Delayed Treatment | 8% |
| 4 | Suicide / Self-Harm | 8% |
| 5 | Retained Surgical Item | 8% |
| 6 | Workplace Violence | 4% |
| 7 | Equipment / Technology Failure | 4% |
| 8 | Medication Errors | 2% |
| 9 | Birth-Related Injury | 2% |
| 10 | Diagnostic Errors | 2% |
| 11 | Pressure Injuries | <2% |
| 12 | Infection-Related Events | <2% |
| 13 | Venous Thromboembolism (VTE) | <2% |
| 14 | Restraint-Related Events | <2% |
| 15 | Elopement | <2% |
| 16 | Infant Abduction / Wrong Discharge | <2% |
| 17 | Anesthesia-Related Events | <2% |
| 18 | Environment of Care Events | <2% |
1). Patient Falls – 49%
During 2024, patient falls resulting in significant injury remained the leading type of sentinel event, accounting for approximately 49% of all sentinel events reported. Patient falls frequently occur when a patient attempts to exit the bed without assistance, or when safety railings are not utilized appropriately.
How to Prevent Patient Falls as Sentinel Events:
- Keep the call bell within reach
- Use non-slip socks and bed alarms
- Check on high-risk patients more often
- Keep floors dry and remove obstacles
- Help patients walk even if they say they are “okay”
2). Wrong-Site Surgery – 8%
Another serious type of sentinel event reported in 2024 was the performance of surgery on the wrong side of the body. Examples of wrong-site surgery include performing surgery on the left knee instead of the right knee. Wrong-site surgery accounts for approximately 8% of sentinel events reported in 2024 and typically occurs due to poor communication or failure to complete verification procedures prior to surgery.
How to Prevent Wrong Site Surgery Event:
- Clearly mark the correct body part before surgery
- Use a “time-out” check where the entire team confirms details
- Match the chart, patient ID band, and surgical plan
- Reduce distractions in the operating room
3). Delayed Treatment – 8%
Delay in treating a condition can result in serious harm to the patient. It can result in stroke victims experiencing permanent damage to the brain. Delayed treatment was the cause of nearly 8% of the sentinel events reported in 2024.
How to Prevent Delayed Treatment as Sentinel Events:
- Educate staff to recognize symptoms of emergent conditions rapidly.
- Develop rapid treatment protocols for serious cases.
- Establish specific timeframes for completion of testing and treatment.
- Provide additional personnel during peak hours.
4). Suicide or Self Harm – 8%
Unfortunately, there were continuing reports of suicidal behavior and self-inflicted injuries in healthcare settings. Suicidal behavior or injuries frequently occur when at-risk patients are not adequately monitored or when safety checks are omitted. Self harm injuries represented approximately 8% of sentinel events reported in 2024.
How to Prevent Suicide or Self Harm as Sentinel Events:
- Use special safe rooms for high-risk patients
- Check rooms carefully for sharp or dangerous items
- Watch at-risk patients closely
- Train staff to spot emotional warning signs
5). Retained Surgical Item – 8%
Although surgical teams are meticulous in counting instruments and supplies during operative procedures, retained surgical item incidents continue to occur. Retained surgical items can lead to postoperative pain, infections and additional surgical interventions. Retained surgical items were the cause of approximately 8% of sentinel events reported in 2024.
How to Prevent Retained Surgical Item as Sentinel Events:
- Use surgical sponges with barcode or radio frequency identification tags.
- Count surgical instruments/supplies prior to, during and after operative procedures.
- Ensure a clean, organized operative field.
- Assign one individual to be responsible for counting surgical instruments/supplies.
6). Workplace Violence – 4%
Healthcare providers were subjected to increasing numbers of violent acts by patients and visitors. Workplace violence has resulted in both physical and emotional harm to healthcare providers and has disrupted delivery of care to other patients. Approximately 4% of reported sentinel events involved workplace violence against healthcare providers.
How to Prevent Workplace Violence as Sentinel Events:
- Educate staff in de-escalation techniques.
- Enhance security measures in high-risk areas.
- Improve communication with anxious patients.
- Design patient-care areas with safe escape routes for staff.
7). Equipment or Technology Failure – 4%
Equipment failures and technology malfunctions during treatment resulted in several sentinel events in 2024 and 2025. The events can include unexpected failure of mechanical ventilation, malfunctioning of monitors and inaccurate readings. Approximately 4% of sentinel events reported in 2024 were the result of equipment failures and technology malfunctions.
How to Prevent Equipment/Technology Failure as Sentinel Events:
- Daily test equipment.
- Timely replace old equipment with new.
- Have backup equipment available.
- Provide education on each piece of equipment for staff.
8). Medication Errors – 2%
Medication errors represent the third most common type of sentinel event reported in the previous year, and account for approximately 2% of all sentinel events. The errors include administering the wrong medication to the patient, administering the wrong dose of medication to the patient, and administering medications to the patient in the wrong order. Some patients experience serious adverse effects due to medication errors.
How to Prevent Medication Errors as Sentinel Events:
- Double-check all medications administered to the patient utilizing the “5 Rights”:
- The Right Patient;
- The Right Drug;
- The Right Dose;
- The Right Time; and
- The Right Route.
- Use bar-code scanning.
- List all of the patient’s known allergic reactions to drugs.
- Limit handwriting when possible.
9). Birth Related Injury – 2%
There were several reports of sentinel events that involved birth-related injuries, including birth-related hypoxia and prolonged labor. Hypoxia and prolonged labor can result in serious injury to newborns. Birth-related injuries were the cause of nearly 2% of sentinel events reported in 2024.
How to Prevent Birth-Related Injury as Sentinel Events:
- Continuously monitor fetal heart rate.
- Summon a specialist early when issues arise.
- Establish birthing emergency teams.
- Promptly decide on a C-section when indicated.
10). Diagnostic Error – 2%
Diagnostic errors happened when a disease was missed or identified too late. As a result, the patient became sicker before receiving the right care. Diagnostic mistakes made up about 2% of sentinel events in 2024.
How to Prevent Diagnostic Errors as Sentinel Events:
- Promote second opinions and follow-up testing.
- Use checklists for common conditions.
- Enhance communication between physicians and laboratories.
- Direct patients to self-monitor symptoms.
Other Less Frequently Reported Sentinel Events in 2024 and 2025
In addition to the commonly discussed sentinel events in 2024 and 2025, the Joint Commission also identifies other serious but less frequently reported events that are 1443 and counting. They are:
11). Pressure Injuries
Pressure injuries, also known as severe pressure ulcers, occur when prolonged pressure on the skin and underlying tissue causes harm to the patient. Pressure injuries can cause permanent damage if not prevented. These injuries include sentinel events because they indicate failures in patient monitoring and care.
How to Prevent Pressure Injuries as Sentinel Events:
- Regularly reposition patients who are immovable.
- Use pressure-relieving mattresses and cushions.
- Perform everyday skin assessments.
- Educate staff and caregivers on proper patient handling techniques.
12). Infection-Related Sentinel Events
Healthcare-associated infections can result in sentinel events as it can cause serious harm or death of the patients. These infections may occur due to lapses in sterile technique, improper hand hygiene, or delayed recognition of infection signs.
How to Prevent Infection-Related Sentinel Events:
- Follow strict hand hygiene protocols.
- Maintain sterile technique during procedures.
- Monitor patients for early signs of infection to avoid harm.
- Implement timely interventions and antibiotic stewardship programs.
13). Venous Thromboembolism (VTE)
VTE, which includes blood clots in veins that may travel to the lungs (pulmonary embolism), is a preventable sentinel event. These events often occur when patients do not receive proper risk assessment or prophylaxis during their ongoing care.
How to Prevent VTE as Sentinel Events:
- Assess patient risk for clot formation on admission.
- Use prophylactic medications or mechanical devices.
- Educate staff and patients on VTE risk factors and symptoms.
14). Restraint-Related Events
Improper use of physical or chemical restraints can cause temporary harm, permanent injury or death. Sentinel events in this category usually involve patient harm due to lack of monitoring or inappropriate restraints application.
How to Prevent Restraint-Related Events:
- Use restraints only when necessary.
- Continuously monitor restrained patients.
- Train staff in safe restraint application and removal.
- Explore alternatives before applying restraints.
15). Elopement
Elopement occurs when a patient leaves the healthcare facility unsafely, leading to potential harm or death of the patients. This is particularly concerning for at-risk patients, including those with cognitive impairments.
How to Prevent Elopement as Sentinel Events:
- Implement secure facility access and monitoring.
- Educate staff on high-risk patient identification.
- Conduct regular patient checks.
- Use electronic monitoring systems when appropriate.
16). Infant Abduction / Discharge to the Wrong Family
Infant abduction or accidental discharge to the wrong family can result in harsh and unpleasant circumstances. These events are sentinel because they indicate critical security and identification failures in the maternity units.
How to Prevent Infant Abduction / Wrong Discharge:
- Use secure identification bands for infants and parents.
- Control and monitor access to maternity units.
- Educate staff on proper verification protocols.
- Implement electronic security alerts for unauthorized movement.
17). Anesthesia-Related Events
Sentinel events can occur when anesthesia administration or monitoring fails. These events often involve airway compromise, overdose, or inadequate patient monitoring.
How to Prevent Anesthesia-Related Sentinel Events:
- Follow strict anesthesia safety protocols.
- Monitor patients continuously during anesthesia.
- Conduct equipment checks before every procedure.
- Ensure staff are trained in emergency airway management.
18). Environment of Care Events
Unsafe environmental conditions in healthcare facilities, such as wet floors, poor lighting, or hazardous equipment, can lead to serious patient harm.
How to Prevent Environment-Related Sentinel Events:
- Regularly inspect the healthcare facility.
- Keep floors dry and pathways clear.
- Ensure proper maintenance of medical equipment.
- Educate staff on environmental safety awareness.
Various Categories of Sentinel Events Occurred In 2025
While sentinel events vary in type, the Joint Commission groups them into several core categories that help healthcare organizations analyze patterns and strengthen patient safety systems.
From 2020 to 2025, the sentinel events occurred are categorized in six categories. In these categories, as per the Joint commission’s report, the top 3 reported the most sentinel events. Care Management Events, Surgical or Invasive Procedure Events, and Protection Events resulted in 4175, 1200, and 621 sentinel events respectively.
Care Management Events
Care management events are among the most frequently reported sentinel event categories and often involve patient falls and delayed treatment.
- Patient falls with serious injury
- Delay in treatment
- Medication management errors
- Infection-related events
- Pressure injuries
- Venous thromboembolism (VTE)
- Perinatal events
- Clinical alarm response failures
- Restraint-related events
- Transition-of-care failures
Surgical or Invasive Procedure Events
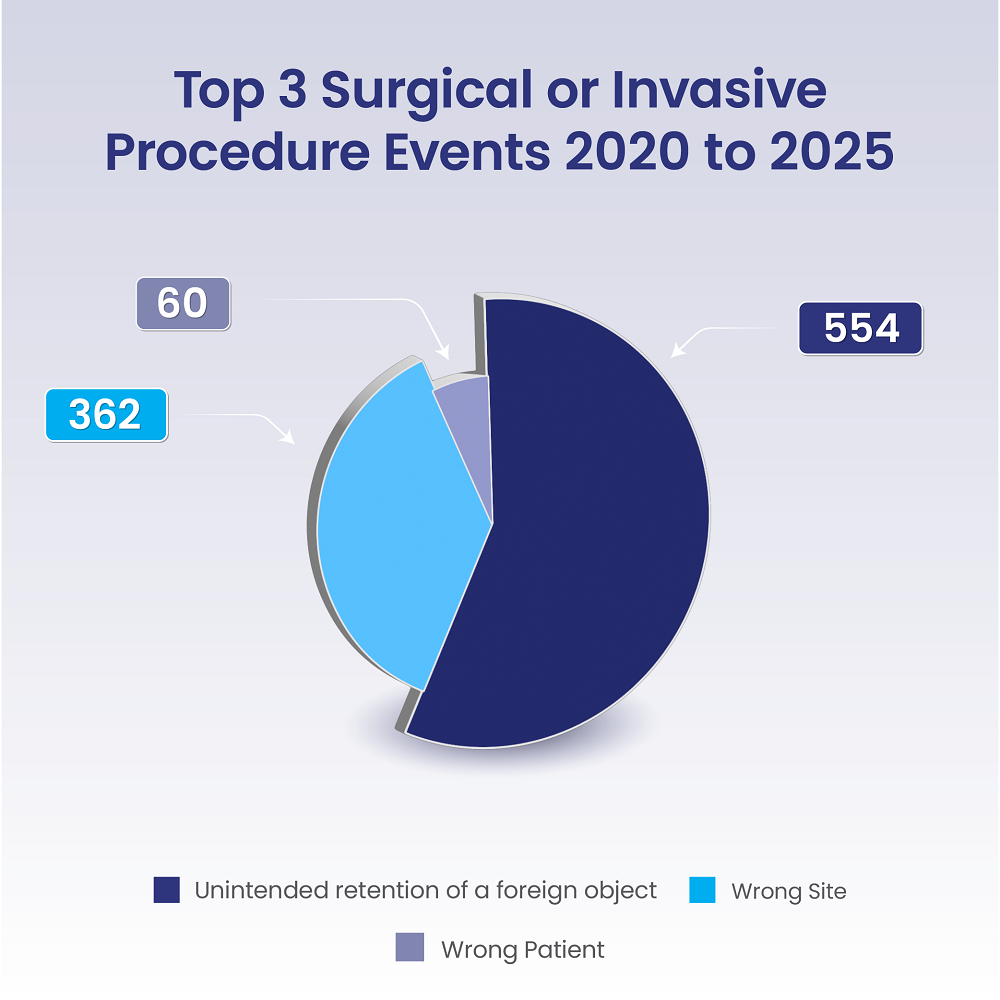
Surgical or Invasive Procedure Events occur before, during, or after a surgical or invasive procedure and often involve verification or communication failures.
- Unintended retention of a foreign object (retained surgical item)
- Wrong-site surgery
- Wrong-procedure surgery
- Wrong-patient surgery
- Wrong implant
- Operative or post-operative complications
- Surgical burns
Protection Events
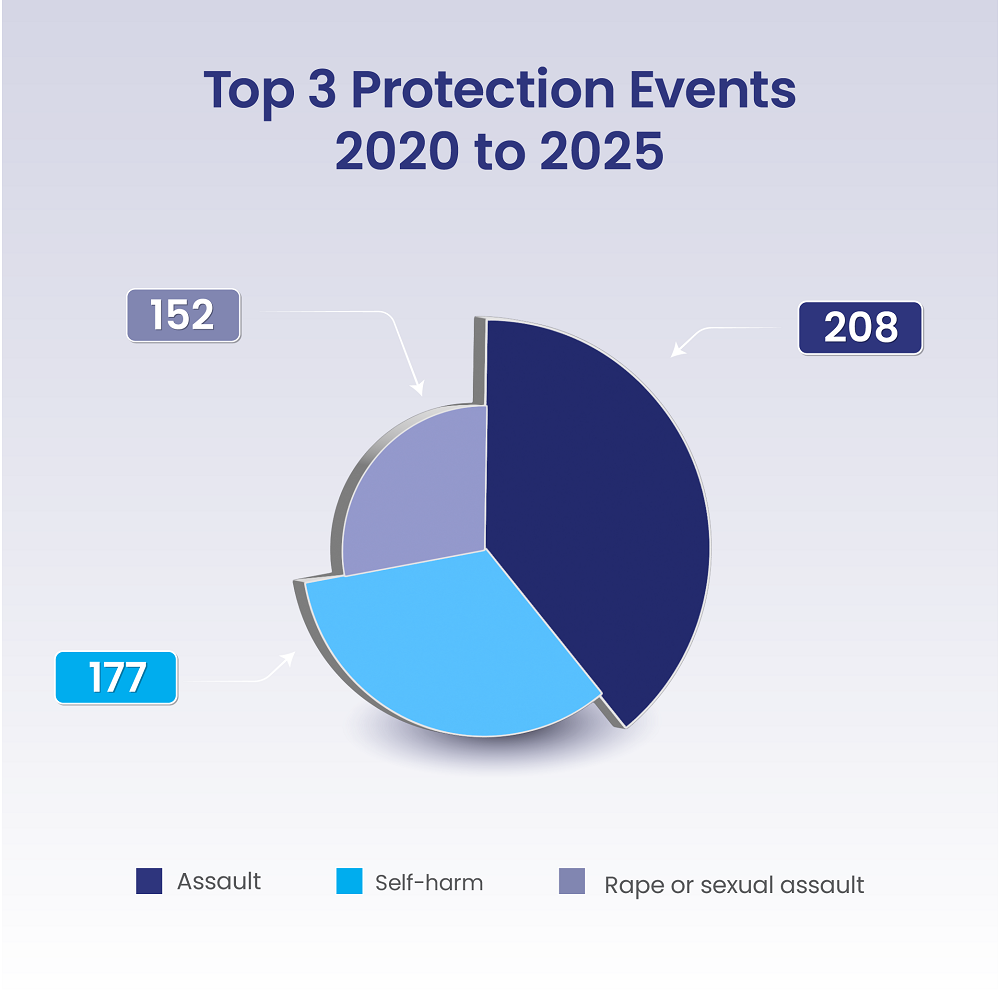
Protection events are serious incidents affecting patient or staff safety and often include assault, self-harm, suicide, elopement, and infant abduction or discharge to the wrong family.
- Assault (including workplace violence)
- Suicide – inpatient
- Suicide – emergency department
- Suicide – offsite
- Self-harm
- Elopement
- Infant abduction
- Infant discharge to the wrong family
- Homicide
- Rape or sexual assault
Anesthesia-Related Events
Anesthesia-related category include less common sentinel events. The sentinel events can cause severe temporary or permanent harm and often involve airway complications, medication errors during anesthesia, or inadequate patient monitoring.
- Airway compromise
- Inadequate monitoring during sedation
- Medication overdose during anesthesia
Product or Device Events
Product or device sentinel events occur when medical equipment malfunctions or is used incorrectly by healthcare staff, and often involve mechanical failures, technology errors, or improper use of medical devices.
- Equipment failure
- Device misuse
- Technology malfunctions affecting patient monitoring or treatment
Environment of Care Events
Environment of care events arise from unsafe physical conditions in healthcare settings and often involve hazards in patient rooms, slippery floors, or other environmental risks leading to injury.
- Slips and falls due to environmental hazards
- Unsafe facility conditions contributing to injury
The Joint Commission Sentinel Event Policy
The Joint Commission is an accreditation agency that evaluates the quality and safety of healthcare settings. When a sentinel event occurs, the Joint Commission expects the healthcare setting to adhere to a formal process. This process is referred to as the Sentinel Event Policy.
The policy requires the following actions:
1). Report the event.
The first action required by the Joint Commission Sentinel Event Policy is for the healthcare setting to report the sentinel event. Reporting the sentinel event to The Joint Commission is voluntary. However, The Joint Commission encourages reporting of sentinel events as it allows the agency to evaluate trends in sentinel events across the nation.
2). Investigate the cause of the event.
Following the initial reporting of the sentinel event, the healthcare setting must conduct a thorough investigation into the circumstances surrounding the event. The investigation should involve:
- Talking to the staff members involved in the sentinel event.
- Reviewing the patient’s medical record.
- Examining video or any other relevant evidence of the event (if permitted).
- Evaluating the policies in place at the time of the sentinel event.
- Creating a chronology of events.
The primary focus of the investigation should be to determine the actual events that occurred, rather than assigning fault.
3). Determine the root cause of the event.
The root cause of the event is the underlying cause of the sentinel event. Identifying the root cause will provide the healthcare setting with the necessary information to develop corrective actions to prevent similar events from occurring in the future. Examples of root causes include:
- Communication failures
- Lack of safety training
- Unclear directions for equipment operation
- Insufficient number of staff
- Poorly written physician orders
- Defective equipment
4). Identify a plan to correct the problem.
Once the root cause of the sentinel event has been determined, the healthcare setting must develop a corrective action plan. The plan must include:
- Corrective actions to address the root cause.
- Specific tasks for each employee responsible for implementing the corrective actions.
- Deadline for implementation of the corrective actions.
- Resources required to implement the corrective actions.
For example:
If a patient fell from the bed because the bed alarm did not operate properly, the corrective action plan would require purchasing new alarms and educating employees on how to check the alarm daily.
5). Verify the effectiveness of the plan.
The Joint Commission requires the healthcare setting to continually evaluate the effectiveness of the corrective action plan. To verify the effectiveness of the corrective action plan, the healthcare setting must:
- Track patient outcomes.
- Evaluate if the frequency of sentinel events decreases.
- Review data collected at 30, 60 and 90 days.
- Modify the corrective action plan if it does not demonstrate effectiveness.
The Joint Commission may request documentation that demonstrates improvements have been implemented.
Guidelines for Handling Sentinel Events in Future
Sentinel event guidelines establish clear expectations for healthcare settings to respond to sentinel events in a consistent manner. Consistent response to sentinel events promotes clarity for healthcare professionals during times of stress.
Below is each section described in further detail:
➜ How to report the event
Healthcare settings should address their staff how to report a sentinel event and instruct them to follow these guidelines:
- Who must be notified inside the hospital
- When they must report a sentinel event (usually immediately)
- How to fill out the incident forms
- When to inform the Joint Commission
- What details must be included in incident forms
➜ How to talk with families
Hospitals must communicate honestly and respectfully with the patient and their family when informing them about sentinel events. Here are some instructions to follow:
- When to tell the family (usually the same day)
- What information must be shared
- How to show empathy and compassion with families
- How to answer questions honestly
- How to apologize when appropriate
➜ How to review the problem
Here are some steps to follow when reviewing the sentinel event and identifying whether it was actually a sentinel event, and then reporting the event.
- Collecting all facts
- Interviewing staff
- Studying equipment or tools involved
- Reviewing policies that may have failed
- Creating a timeline of events
- This review must be fair, respectful, and fact-based.

