Medical Billing Services for Healthcare Providers in Houston
Houstonian Physicians Lose Thousands Every Month. BellMedEx Stops That!
Houston Southwest Medical Billing Group by BellMedEx is one of Houston’s top medical billing firms that works with practices tired of seeing revenue disappear into denials, delayed payments, and claims nobody had time to chase properly. Many times, these lost revenues come from missed small things over again like coding errors, wrong modifiers, and incorrect claim submissions. This results in many practice losing 15% to 20% of their claims being rejected on the initial submission.
Houston physician offices can be assured of complete Revenue Cycle Management from BellMedEx as well as all aspects of verification, follow-up on submitted claims, denial resolution and appeals.
We have all of our billers/coders certified to provide medical billing in Houston’s healthcare market. So we know what each payer does locally because it’s not just “what the books say” but also from actual experience.

Request Free RCM Consultancy
CMRS · RHIA · CPB Certified
100% HIPAA Compliant
24/7 Support
Free EHR Software Included
90+ Specialties Covered
Houston-Specific Billing Challenges
We manage the details that make Houston Billing complex
There are 60+ hospitals in Houston and Houston has one of the most diverse insurance markets in the United States with multiple types of health plans such as Medicaid managed care, Medicare advantage, Blue Cross/Blue Shield of Texas (BCBSTX), Aetna, UnitedHealthcare (UHC), Cigna, and numerous other regional managed care organizations (MCO). All have their own rules.
TMHP implemented annual HCPCS updates on January 1, 2026, with additional policy updates and clarifications issued throughout the year
60+
Hospitals in the Houston metro area
Up to 20%
Claims denied on first submission
Multiple Payers
Too many payers, too many rules
3–10%
Revenue lost annually from billing errors
15% to 18%
Uninsured population in Texas

100% Compliant
with Texas Healthcare Industry
97%+
First-pass claim acceptance rate
40+ Payers
Working with All Payers in Texas
15%+
Average revenue increase
25%+
Increase in patient collections
How BellMedEx Helps You
We work as your Full Service Medical Billing Partner in Houston
Our top-rated Houston Medical Billing Company has helped healthcare practices leave behind inefficient billing workflows and transition into more accurate and more reliable billing.
Whether it is an independent family practice or specialist office located in The Heights or West University, or whether you are part of one of the many busy physician specialty groups operating in the Medical Centre of Texas, our company delivers clinical billing solutions built for the pace, payer mix, and reimbursement pressure of the Houston’s whitecoat community.
This top-notch Texas Medical Billing Support makes BellMedEx a go-to partner for healthcare professionals.

Verification of Insurance Coverage
Before every visit, BellMedEx checks each patient's insurance coverage that can significantly reduce the risk of unexpected denials. The team will verify all insurance benefits, copays, deductibles and authorization requirements at the moment the services are rendered.

Coding (CPT, ICD-10, HCPCS)
The medical coding experts at BellMedEx include CMRS, RHIA and CPB certified professionals who track every code update including the 2026 HCPCS updates adopted by Texas Medicaid (TMHP). Your practice does not want incorrect codes to result in lost revenue. Our coding team is trained to maximize first-pass accuracy and minimize errors.

Submission of Clean Claims
Each claim is reviewed before being submitted. We review demographic information, coding, payer edits, and modifier data. This is why you typically receive a 97% clean claim first-pass submission when working with BellMedEx.

Denial Management & Appeals
If an insurer denies a claim, we will investigate each denial, correct errors, and resubmit the claim usually within 24 to 48 hours with supporting documentation. Our goal is for you to collect the funds owed to you. Most other billing companies will not invest time and efforts in this type of follow up.

Provider Credentialing & Enrollment
Houston provider credentialing can take a long time and can also be complicated. BellMedEx manages the application process; license verification; CAQH profile creation; and the management of payor contracts. We have achieved a 98% successful credentialing rate for our partners.

Accounts Receivable (A/R) Follow-Up
Money that sits in aging accounts receivable is uncollected money. BellMedEx tracks the status of submitted claims, contacts the payors, and highlight delayed claims. We help reduce A/R days significantly, with many clients performing well below industry averages (typically 30–50 days)

Texas Medicaid Billing (TMHP)
TMHP has its own set of rules, guidelines, timelines and MCO variations. At BellMedex we understand TMHP procedures including the 2026 Texas Medicaid Provider Procedures Manual updates; the prior authorization process changes; and filing deadlines for each Texas Managed Care Organization.

Free EHR & Billing Software
You get to use whatever platform you like. Or, if you prefer, we can give you access to a free in-office EHR that is built into your Houston Healthcare Billing System. There are no additional software costs or set-up charges associated with this service; simply included in the flat 2.49% collection fee.

Full Revenue Cycle Management (RCM)
Each claim is reviewed before being submitted. We review demographic information, coding, payer edits, and modifier data. This is why you typically receive a 97% clean claim first-pass submission when working with BellMedEx's Houston Medical Billing Solutions.
Specialties We Serve in Houston, TX
Your Specialty. Your Payers. Our Expertise.
Family Medicine
Internal Medicine
Cardiology
Orthopedics
Neurology
Dermatology
Behavioral Health
Mental Health / Psychiatry
Urgent Care
OB/GYN
Pediatrics
Oncology
Urology
Gastroenterology
Ophthalmology
Radiology
Physical Therapy
Chiropractic
Pain Management
Anesthesia
Emergency Medicine
Rheumatology
Pulmonology
Surgery
Endocrinology
Podiatry
Nephrology
+ 63 More Specialties
Here’s how BellMedEx shines in comparison with other Houston Billing Companies
| BellMedEx vs. Other Houston Billing Companies | |||
|---|---|---|---|
| Feature |  |  | |
| Pay-for-Paid Model | Yes — always | Not confirmed | Varies by plan |
| Transparent Starting Rate | From 2.49% | Not public | Not public |
| Free EHR Software Included | Yes — free | No | No |
| Clean Claim Rate | 97%+ | Not disclosed | Not disclosed |
| Certified Coders (CMRS/RHIA/CPB) | Every claim | Yes | Partial |
| Number of Specialties Covered | 90+ specialties | Limited range | 20 specialties |
| 2026 TMHP / Texas Medicaid Updates | Real-time tracking | Manual updates | Manual updates |
| Free Denied Claims Appeals | Always included free | Extra cost | Varies |
| 24/7 Support | 24/7 | Business hours only | Business hours only |
| Real-Time Billing Dashboard | Full dashboard included | Limited reporting | Yes |
| Verified Public Reviews (4.8+ Stars) | 350+ verified reviews | Limited online reviews | Limited online reviews |
| Full Credentialing Included | Yes — full service | Yes | Add-on cost |
Note
= Confirmed available
= Not available
= Partial or unconfirmed based on publicly available data
The Medical Billing Company that Houston Practices use across major carriers
The details about insurance coverage and payment by payers can be very confusing due to how many payers there are in Houston. As an example, patients may have over a dozen insurance policies and each will have its own way of doing things such as what type of information they require before authorizing a treatment; or which types of treatments they will cover and at what level. All of these differences make it difficult for doctors to find ways to bill and get paid for services provided.
At BellMedEx, our team handles billing and payments for major payers across the Houston Provider Network and also provides additional support for payers not listed below.












Available Across Houston
As Houston’s favorite Medical Billing Services Company for hospitals and physicians across the Bayou City and the wider Houston metro, we know the local healthcare market from the Texas Medical Center out to the fast-growing suburban practice corridors. We support you with Houston-specific Healthcare RCM Services shaped around how reimbursement, payer behavior, and practice operations actually work in this part of Texas.
- Texas Medical Center and Inner Loop practices
- The Heights and River Oaks clinics
- Memorial and Galleria-area medical offices
- Katy, Sugar Land, and Pearland groups
- Pasadena, Clear Lake, and Bay Area Houston providers
- Spring and The Woodlands healthcare partners
Affordable Pricing
With our reasonable rates (beginning as low as 2.49% of your monthly collections), pay-for-paid approach, free EMR software, integrated scalability, and free denied-claim appeals support, you may save money compared to in-house billing. Contract with us to optimize your billing with benefits like:
- Billing Software
- Denial Management
- Accounts Management
- Electronic Statements
- Clearinghouse Services
- 1:1 Technical Support
In-House Billing Costs
| In-House Billing Costs | |
|---|---|
| *calculations based on a medium-scale practice with $100,000 collections | |
| Annual Salary | $54,480 |
| Overheads | $15,000 |
| Total | $69,480 |
BellMedEx Full Service Medical Billing Costs
| BellMedEx Full Service Medical Billing Costs | |
|---|---|
| *calculations based on a medium-scale practice with $100,000 collections | |
| Billing Service Rates | as low as 2.99% of the collections |
| Total | $35,998 |
Annual Savings with BellMedEx
| Annual Savings with BellMedEx | |
|---|---|
| $33,482 |
2026 Updates
Texas Medical Billing changed in 2026 and BellMedEx delivers for Houston Providers
Houston providers need to know about these changes or risk denied claims and lost revenue.
Active 2026 HCPCS codes for all of Texas available from TMHP
TMHP activated their full 2026 HCPCS coding update effective January 1. Many of the older codes were removed attempting to bill those codes today will result in an auto denial by TMHP. In addition to the removal of existing codes, new codes may not be reimbursed until Medicaid establishes or updates reimbursement rates through its review process. Your staff needs to be current with all coding changes as soon as possible to avoid lost revenue.
Solution:
BellMedEx Houston Billing Experts update your billing system with the latest HCPCS codes to prevent automatic denials of results from using outdated codes.
Reimbursable rates for Texas Medicaid claims changed again
As a direct result of the public rate hearing held in November 2025, new Medicaid Reimbursement rates went into effect for all claims dated March 1, 2026 or later. The reimbursement rate change impacts a number of areas including; hearing aids, musculoskeletal surgery, radiology, and surgical procedures related to the male genital system. Any practice that continues to use the old rates for claims billed after March 1st will likely receive less than what they deserve and may not even realize it.
Solution:
BellMedEx will review your claims against the most recent TMHP Reimbursement Rate to ensure you are being paid the full allowed amount. If the rate increases, we will automatically update your billing submissions.
BCBSTX cut prior auth response times — but added new reviews
The prior authorization process for Medicare advantage patients from Blue Cross Blue Shield of texas began moving faster. However, physicians who are exempt from prior authorizations under HB 3812 will now find themselves being reviewed by BCBSTX for compliance. Providers who do not maintain at least 90% approval rate for prior authorization requests may lose their exemption status and be required to resume standard prior authorization processes.
Solution:
By maintaining low error rates (below those set by auditors), we help you maintain your exemption status and reduce the likelihood of an unexpected slow down or delay in processing claims.
Prior authorization code updates for BCBSTX Medicaid
On April 1, 2026 Blue Cross Blue Shield of TX implemented new prior authorization code lists for its Medicaid members. Should your billing team fail to obtain the updated prior authorization list, anticipate an immediate increase in denied claims. Clients of BellMedEx currently have this information updated and available.
Solution:
The BellMedEx team will proactively update your prior authorization code lists before any changes take place. Once the updates occur, our Medical Claims Operations Team will ensure your staff understands what is required to process claims efficiently to minimize the number of denied claims.
Novitas updated 18 Medicare articles for new CPT/HCPCS codes
In support of the new CPT and HCPCS coding Changes for 2026, Novitas Solutions, the Medicare Administrative Contractor serving Texas, updated 18 billing articles. Modifier 25 remains valid, but improper or unsupported use especially for same-day E/M services with procedures may trigger payment reviews, denials, or audits. This issue is particularly relevant across the Houston Multi-Specialty Practice Network.
Solution:
The BellMedEx team will identify and address any incorrect modifier usage prior to submitting your claims. With fewer errors in your claims, you will experience less risk of having your claims audited and reduced lost revenue.
Texas Medicaid MCO filing deadlines vary
Each of the various managed care organizations (MCOs) participating in Texas Medicaid have different time limits for timely filings. Molina Texas Medicaid has a 90-day window. Medicare has a 12-month window. Commercial payers vary based on the terms of your contract. Missing filing deadlines can significantly reduce the likelihood of reimbursement, though appeals may still be possible in certain cases.
Solution:
BellMedEx tracks filing deadlines across the Houston Payer Landscape and ensures timely claim submission. We automate alerts and workflows stopping revenue slips through the cracks. This prevents irreversible revenue loss from missed deadlines.
Real Results
Testimonials

Internal Specialist Medicine
What helped us with BellMedEx was they understood our billing needs pretty much right away. Coding was getting checked properly and the patient invoicing side stopped feeling like something we were always behind on.

We had used other medical billing services before, but Houston Southwest Medical Billing Group felt different from the jump. They got into the billing and coding details and made the whole patient billing process feel a lot less heavy on my team.

Orthopedic Surgeon
Around Houston, you can tell quick who really understands billing needs and who is just talking. BellMedEx helped us tighten up patient insurance invoicing without making everything more complicated for the office staff.
Our Medical Billing Software is built for Healthcare Practices in Houston
A number of medical billing systems appear functional when you are creating invoices. However, this is typically when billing problems begin to occur. The most common billing problem experienced by Houston physicians is payer variation or authorizations which causes claims to be rejected by a payer. BellMedex’s Houston Revenue Cycle Platform streamlines these various elements into a single software application and establishes workflows based upon how the Houston payers process their claims. Therefore, if the patient is assigned to Blue Cross Blue Shield of Texas (BCBSTX), the clearinghouse will not send that claim as though it is intended for all payers. Rather, it is sent to BCBSTX. Same with Texas Medicaid and TMHP. This is generally where cleaner claims originate.
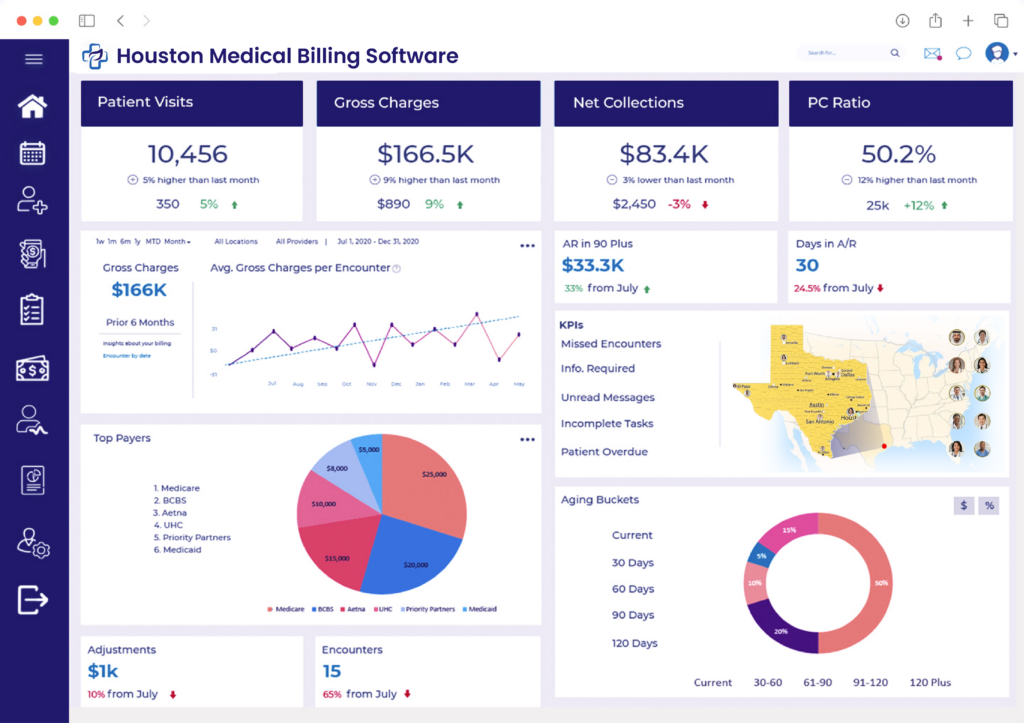
Built Around Texas Payers Logic
BellMedEx’s billing software utilizes the same payer-specific logic that many physicians practicing in Houston experience on an everyday basis rather than utilizing a one size fits all approach to processing each claim.

Flow Based Upon Paying Insurer
Once the physician identifies the insurer associated with the patient, BellMedEx’s software processes the claim as such prior to sending it from the provider’s office.

Less Time Spent Fixing Claims on Back End
As previously stated, cleaner claims reduce the amount of time spent by the clinician’s in-house staff correcting issues related to denied claims.
FAQs
Frequently Asked Questions
What does Houston Southwest Medical Billing Group do?
Houston Southwest Medical Billing Group is a subsidiary of BellMedEx that handles every step of the billing cycle so you don’t have to spend precious hours chasing payers. Our team reviews and scrubs every claim for errors, verifying even the smallest technical details before submission. We then track each claim throughout its lifecycle until it is paid. If a denial occurs, we manage the entire appeal process to help you secure full reimbursement.
In a complex market like Houston, local payer rules and portal issues can delay or stall claims without warning. We handle everything from accurate documentation and precise coding to payer-specific claim submission and timely payment posting, so you avoid revenue loss and get paid correctly, on time.
How is outsourced billing different from in-house billing?
Managing billing in-house works for some groups. It gives them control and allows for better communication. Most practices rely on one or two experienced people who know the system, like what to handle, what to leave alone, which payer needs a call, and which one just takes time.
The real problem begins when those people leave, are overburdened, or pulled into other important tasks. Although everything seems normal, the claims get processed every day, but cash flow becomes unpredictable. This is where outsourced billing saves the day. Partnering with an experienced RCM company allows you to leverage a dedicated team of highly skilled and focused professionals who ensure consistent revenue and financial integrity.
What areas of Houston do you cover?
We serve providers across the entire Greater Houston metro — Texas Medical Center, Katy, Sugar Land, The Woodlands, Pearland, Pasadena, Baytown, Friendswood, and surrounding areas. Since our service is remote, we can also serve any Texas provider statewide.
How will you handle denials or delayed payments?
Denials and delays are not best evaluated solely by reviewing reports. Rather, we review each denial/delayed payment to determine the causes.
- Was it coding errors?
Edit errors? - Lack of supporting documentation?
- Eligibility issues?
- Were claims filed incorrectly?
- Were delays caused by a particular payer's processing practices?
- Were delays caused by a lack of timely communication between departments/individuals within your practice?
Once we have identified the root causes of the denial/delayed payment, we develop strategies for resolving them. We directly address the underlying reason for the delay.
Can I see how my billing operation is performing?
Yes, you will be able to view key performance indicators related to your billing operations without having to interpret data. The KPIs we provide, include metrics (in an easy-to-understand format) such as:
- which accounts receivable are being aged longer than others?
- are certain types of claims consistently denied or rejected?
- is there a concentration of denials/rejections among specific payers or types of services?
- are collections improving or merely artificially supported by past AR balances?
We believe that monthly or weekly reporting should reduce confusion and create clarity regarding operational effectiveness. Ideally it should eliminate the need for additional meetings, and that is the standard we aim for.
Do you support advanced or specialty medical billing?
Yes. In Texas, a lot of medical groups have to do more than just make claims for their patients. Many billers (who work without local market context) don't know all the details that go into specialized billing, like carefully going over all the paperwork that pertains to each patient's care, handling denials before they become a problem, taking specific steps to communicate with payers, and always keeping track of the payment status to find out where patient revenues are being held up. In a market this layered, things slip through more easily than they should. That’s one reason we’re here!
Sign up and book a free service demo
Choose the best package for your practice
Service Type | Medical Billing Services |
| Provider | BellMedEx |
| Subsidiary | Houston Southwest Medical Billing Group |
| Specialties Served | Family medicine clinics, internal medicine practices, orthopedic groups, cardiology offices, pain management clinics, behavioral health centers, and outpatient care providers |
| Service Price | as low as 2.49% of your monthly collections |
| Location | Houston Southwest Medical Billing Group office, P.O. Box 77002, Houston, TX |
| Contact Number | 888-987-6250 |
| Business Hours | Mon–Fri: 8 AM – 6 PM (CST) |
© Bellmedex 2026 All Rights Reserved.
